Allergy
Blood Diseases
Bone & Joints
Brain
Cancer
Child Care
Cosmetic Surgery
Diabetes
Endocrinology
ENT
Eye
Gen Medicine
General Surgery
Heart
Kidney
Lifestyle
Liver & Digestive
Lung
Men’s Health
Mental health
Physiotherapy
Rheumatology
Skin and hair
Sleep Disorders
Spine
Transplant
Women Health
Thyroid
Vascular Surgery
Psoriasis
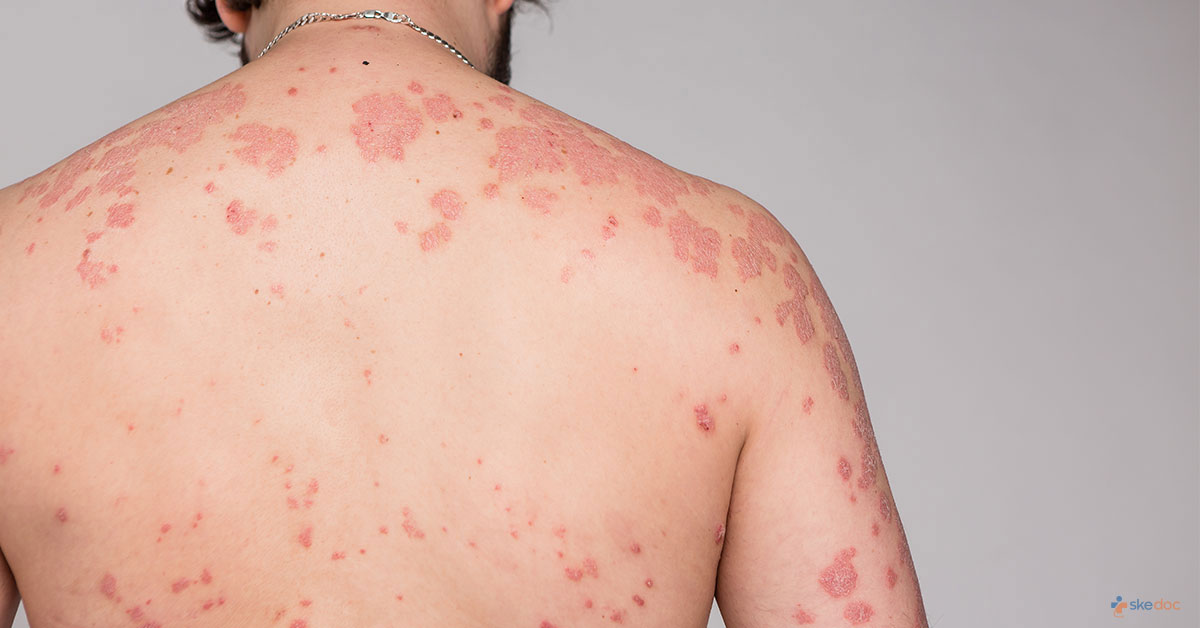
What Is Psoriasis?
Psoriasis is a long term non-contagious disease of the skin that presents as abnormal patches. Multiple factors such as genetics, environment, and the immune system cause the cells of the skin to multiply rapidly, resulting in dry, scaly, red, and itchy areas of raised regions on the skin at the elbows, knees, and the scalp, between the buttocks, on the back, and sometimes on the nails, and the glans penis as well.
Is this condition a medical emergency?
Psoriasis is not a medical emergency.
Types of psoriasis
Psoriasis can be seen as one of the following types:
- Chronic stationary psoriasis: Seen on the scalp, genitals, outside surfaces of the joints, umbilicus, lower back, and behind the ears.
- Plaque psoriasis: Seen on the upper surface of the knees and elbows, scalp, and the trunk.
- Guttate psoriasis: Mostly seen on the trunk, appearing suddenly after a respiratory infection and appearing as water drop shaped scaling patches.
- Inverse psoriasis: Seen on the armpits, back of the knee, under the breasts, the groin, and skin folds.
- Pustular psoriasis: Usually seen on the palms or the soles, or sometimes all over the body, and presents as pus-filled blisters that appear a few hours after the skin turns red.
- Erythrodermic psoriasis: Seen on the entire body with reddish skin and scales that peel off.
- Scalp psoriasis: Seen on the scalp.
- Nail psoriasis: Appears similar to fungal nail infections.
- Psoriatic arthritis: Affects the joints of the hands and the feet and sometimes the large joints.
- Oral psoriasis
- Eruptive psoriasis: Mostly affects the younger age group, and is seen on the upper part of the trunk and the arms.
- Napkin psoriasis: Affects the diaper region.
- Linear psoriasis: Seen affecting a region of the skin supplied by a single spinal sensory nerve.
Causes of psoriasis
The exact cause of psoriasis is not fully understood, but it has been observed that the T cells and neutrophils which are a part of the body’s immune system mistakenly attack the skin cells, and this, in turn, causes more skin cells to be produced in response at a much faster rate of 3-5 days rather than the normal 25-30 days, and this process keeps repeating over and over. The inflammation that is produced as a result of the immune system activity results in the redness, itching, and warmth of the psoriasis patches.
Risk factors
The risk factors for developing psoriasis include:
- Family History
- Infections especially Strep throat and HIV
- Obesity
- Stress
- Smoking
- Dry skin
- Medications such as beta-blockers, NSAIDs, lipid-lowering medications, antimalarials, withdrawal of corticosteroids
Triggering factors
The triggers for psoriasis may include:
- Infections
- Smoking
- Stress
- Vitamin D deficiency
- Excessive alcohol consumption
- Injuries to the skin such as cuts and bites
- Climate change
Symptoms & signs of psoriasis
The symptoms and signs of psoriasis include:
- Red patches of skin covered with silvery scales
- Small spots that scale
- Dry and cracked skin that may bleed
- Itching
- Burning or soreness
- Swollen and stiff joints
- Pus filled blisters
Investigations
There are no investigations that are specifically needed for this disease, but the following may be done to rule out other conditions
- Laboratory tests-
- CBP and ESR
- Rheumatoid factor
- Uric acid levels
- Fungal studies
- Skin Biopsy: Punch Biopsy
- X-ray Joints: To evaluate joint involvement in psoriatic arthritis
- Bone scans: For early identification of joint involvement
Diagnosis of psoriasis
The diagnosis of psoriasis is established based on medical history and clinical evaluation and the results of the investigations done. Epidermal thickening and clubbed epidermal projections are diagnostic of this disease on histopathological examination of the biopsied skin.
Psoriasis treatment options
There is no cure for this disease, but the condition can be managed with medication based on its severity.
A. Medical management
The medical management of psoriasis includes:
- Topical Therapy
- Topical Steroids: To reduce inflammation and reduce itching.
- Vitamin D analogs: To slow skin cell growth, and usually used in combination with steroids.
- Anthralin: To slow skin cell growth and remove scales.
- Calcineurin inhibitors: Such as tacrolimus to reduce inflammation and plaque build-up.
- Salicylic acid: To reduce scaling.
- Coal tar: To reduce scaling, itching, and inflammation. Not recommended for pregnant or lactating women.
- Moisturizers: To reduce itching, dryness, and scaling.
- Systemic therapy
- Retinoids: Indicated in severe psoriasis not responding to other therapies. (Women who are taking retinoids need to avoid getting pregnant for at least 3 years after stopping the medication, to avoid birth defects).
- Methotrexate: Slow skin cell production and reduce inflammation by suppressing the immune system.
- Cyclosporine: To reduce inflammation by suppressing the immune system.
- Monoclonal antibodies: A new class of drugs such as Infliximab, Adalimumab, etc., that suppress the actions of the immune system.
- Phototherapy: Light therapy
- Sunlight: Exposure to sunlight for short periods at a time can help to reduce skin cell turnover. Long periods of exposure can worsen
- UVB phototherapy or Broadband UVB phototherapy: Effective in mild to moderate this disease, controlled doses of Ultraviolet light from an artificial light source are given.
- Narrowband UVB phototherapy (NBUVB): The artificial light source emits a narrower band of UV light than the one seen in broadband UVB.
- Psoralen plus ultraviolet A (PUVA): Indicated in severe cases, and uses a combination of Ultraviolet A light in combination with a chemical called psoralen which makes the skin more responsive to UV A light.
- Excimer Laser: Indicated in mild to moderate psoriasis, and uses a high-intensity UV Blight that is focused only on the plaques and sparing the surrounding unaffected skin.
B. Role of diet/exercise/lifestyle changes/preventive measures
Some measures that can help to control this disease include:
- Bathing everyday
- Avoiding smoking and alcohol
- Getting sunlight exposure regularly for a short duration
- Keeping skin soft and moist by using a moisturizer
- Avoiding any known triggers that aggravate the condition
Complications
There can be several complications that can arise or are more common in individuals with this disease. They include:
- Psoriatic arthritis
- Diabetes type 2
- High blood pressure
- Heart disease
- Obesity
- Metabolic Syndrome
- Kidney disease
- Eye conditions such as conjunctivitis, blepharitis
- Parkinson’s disease
- Depression and low self-esteem
Prognosis
The prognosis for this disease is generally good, and most individuals with mild to moderate psoriasis respond well to treatment. However, it can affect the quality of life, and also predispose to more serious conditions such as heart disease, kidney disease, and diabetes, and these conditions may lead to early mortality when compared to individuals without psoriasis.
When to contact the doctor or hospital/How to identify the emergency or complications?
This disease does not lead to any medical emergencies but it is advisable to consult a medical expert when any skin conditions that are present are worsening, changing, or not responding to management as they should.
Indications for hospitalization if required
Hospitalization is not required.
Screening methods
Individuals with this disease are advised to get themselves screened for Psoriatic Arthritis every year using the psoriasis Epidemiology Scoring Tool (PEST) method.
Suggested clinical specialist/Departments to consult for this condition
This Disease will be treated by specialists from the Department of Dermatology.
Was this article helpful?
YesNo




