Allergy
Blood Diseases
Bone & Joints
Brain
Cancer
Child Care
Cosmetic Surgery
Diabetes
Endocrinology
ENT
Eye
Gen Medicine
General Surgery
Heart
Kidney
Lifestyle
Liver & Digestive
Lung
Men’s Health
Mental health
Physiotherapy
Rheumatology
Skin and hair
Sleep Disorders
Spine
Transplant
Women Health
Thyroid
Vascular Surgery
Pemphigus
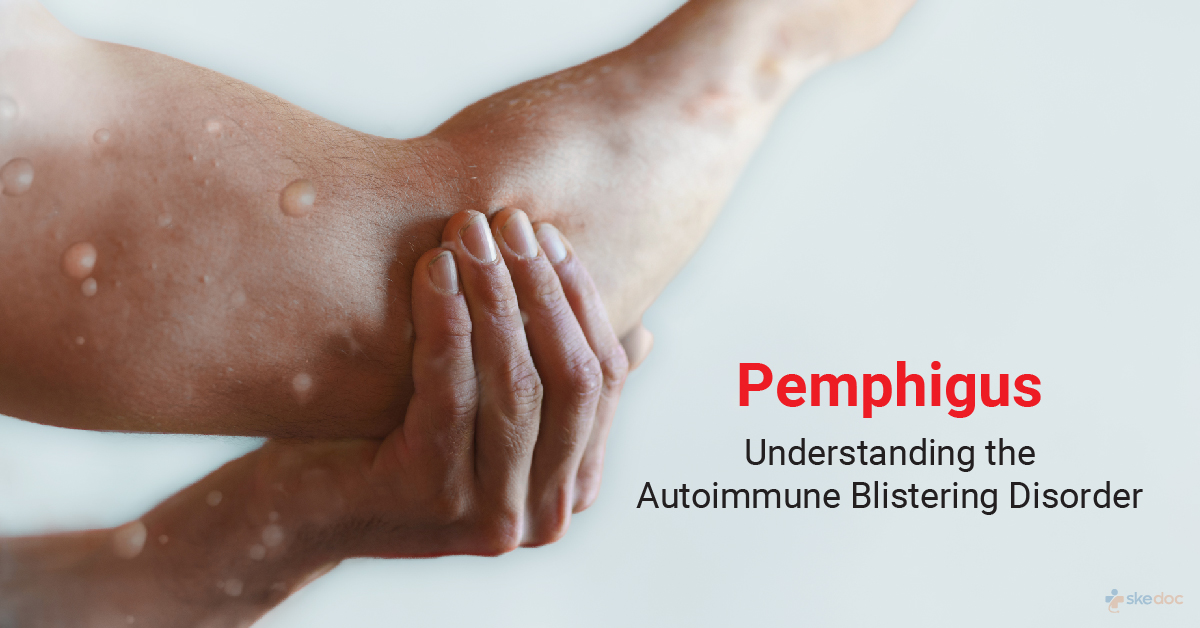
What Is Pemphigus?
Pemphigus is an autoimmune disease of the skin and the mucous membranes (linings of the mouth, eyes, nose, genitals, etc.) that results in painful blisters with erosions. It is a condition that persists for a very long time and mostly affects middle-aged and elderly individuals.
Is this condition a medical emergency?
It is not a medical emergency, but untreated and can lead to life-threatening complications.
Types of Pemphigus
It may be of the following types, with the first four being the most common
- Pemphigus Vulgaris: It is the most common type, with the blisters originating in the mouth
- Pemphigus foliaceus: It is the least severe of all varieties of pemphigus and does not usually affect the mucus membranes
- IgA pemphigus: Due to the presence of circulating IgA antibodies as opposed to IgG antibodies in most other types of pemphigus,
- Sub corneal pustular dermatosis type IgA (SPD-IgA)
- Intraepidermal Neutrophilic type IgA (IEN-IgA)
- Paraneoplastic Pemphigus: Associated with an underlying tumor
- Drug-Induced Pemphigus: Secondary to the use of thiols or thiol producing drugs
- Pemphigus Erythematosus: It is a localized form of Pemphigus
- Pemphigus Vegetans: It is a localized form of Pemphigus, in which instead of healing, the lesions form papillomatous growths
- Endemic pemphigus foliaceus
Causes
Pemphigus is an autoimmune disease in which the body’s immune system attacks the skin and the mucus membranes. Antibodies such as IgG (most common), IgA, or IgE are produced by the immune system against proteins called desmogleins that help in the cell to cell binding of the epithelial cells of the skin and the mucus membranes. The antibodies attack and destroy the desmoglein proteins, resulting in the separation of the epithelial cells and collection of fluid, leading to acantholysis, resulting in the formation of blisters and skin sloughing.
Risk factors
Some risk factors for Pemphigus include
- Age: The middle-aged and the elderly are at a greater risk
- Race: Indian, Middle-Eastern, and Jewish population is at a greater risk
Triggering factors
Pemphigus may sometimes be triggered by
- Trauma
- Stress
- Infection
- Cancer
- Drugs
- Thiol drugs: Such as Penicillamine, ACE inhibitors (captopril, enalapril)
- Non-Thiol drugs: Penicillins, cephalosporins, antihypertensive agents, piroxicam
Symptoms & signs
The symptoms and signs may depend on the type that is present and include the following
- Pemphigus Vulgaris
- Painful blisters that start in the inside of the mouth (most common) or on the genitals
- Blisters on the skin may or may not develop a few weeks later
- Blisters are thin-walled, flaccid (soft), and filled with clear fluid; the blisters easily rupture
- Once the blisters rupture and cause erosion there is usually severe pain
- Difficulty in eating and swallowing if the blisters are present in the throat
- Hoarseness of voice if the blisters affect the larynx
- The eyes, nose, urethra, anus, vagina, labia, cervix, or penis may be affected
- The skin around the nails may be affected and is red and painful
- Pemphigus foliaceus
- The blisters usually start on the body first such as on the back, chest, or the shoulders
- There is intense itching
- Pain is absent or very minimal
- The mouth is usually not affected
- Pemphigus vegetans
- The blisters form in the skin folds
- After erosion, the blisters do not heal but instead, form growths that have a crusted appearance
Investigations
Some investigations that may be done to establish a diagnosis may include the following
- Laboratory tests
- CBP & ESR
- Basic Metabolic Panel
- ELISA testing of blood or saliva for Anti DSG1 and Anti DSG3 antibody titers
- Skin Biopsy
- Direct Immunofluorescence on normal-appearing skin adjacent to the lesion
- Indirect Immunofluorescence using the individual’s serum if direct Immunofluorescence is positive
- Endoscopy: May be done if lesions are suspected to be present in the throat
Diagnosis
A diagnosis is established based on medical history, clinical evaluation, and the results of the investigations done.
Treatment options
The treatment of Pemphigus aims to decrease blister formation, prevent secondary infections, promote healing of blisters and erosions, and administer the right and minimum dose required to keep the disease under control. The disease responds differently in different individuals. Therefore, the pharmacologic therapy and medication dosage are adjusted according to individual needs.
Medical management
Medical management of Pemphigus includes the following
- Anti-inflammatory agents: Such as prednisone, act by reducing and preventing the inflammatory process initiation by the immune system
- Immunosuppressant agents: Such as azathioprine, methotrexate; are used in addition to anti-inflammatory agents, especially in those who are unable to tolerate high doses
- Anti CD-20 Monoclonal Antibodies: such as Rituximab, Act by suppressing the antigens that trigger an immune response
- Dapsone: Used for its anti-inflammatory properties when corticosteroids are not tolerated
- Hydroxychloroquine: Used for its anti-inflammatory properties when corticosteroids are not tolerated
- Intravenous Immunoglobulins: Act as immunomodulators that reduce the inflammatory response of the body
- Nicotinamide: Used for its anti-inflammatory properties when corticosteroids are not tolerated
- Antibiotic therapy: To prevent bacterial infections; some antibiotics such as tetracyclines help to reduce the severity of the disease
- Calcium supplementation: To prevent osteoporosis especially in women being treated with corticosteroids
Interventional including surgery and indications for surgery
Interventional management of Pemphigus may include
- Extracorporeal Photopheresis
- Plasmapheresis or plasma exchange therapy
Role of Diet/exercise/lifestyle changes/ preventive
Some measures that can be taken to cope with Pemphigus include the following
- Avoid sun exposure
- Proper wound care and management to prevent infections and scarring
- Avoid using harsh soaps for bathing or cleaning
- Avoid spicy and hard food to reduce mucosal irritation in the mouth
- Cessation of any drugs that may be triggering the condition and replacing them with alternative medications
Complications
Some complications that may be seen with Pemphigus include
- Skin infections
- Sepsis
- Malnutrition due to poor diet and inability to eat
- Fluid and Electrolyte imbalances
- Side effects of medications used for treatment such as hypertension, diabetes, liver toxicity
- Death
Prognosis
The prognosis of Pemphigus varies and is generally average with the disease affecting the quality of life. Long-term medication, especially with immunosuppressant agents, can lead to other complications. In general, the prognosis depends on the severity of the disease and the age of the individual with extensive disease and older age having a poorer prognosis.
When to contact the doctor or hospital/how to identify the emergency or complications
It is advisable to seek medical attention if the symptoms and signs are noticed.
Indications for hospitalization if required
Hospitalization will not be required unless severe complications such as sepsis need to be managed.
Suggested clinical specialists/departments to consult for this condition
Specialists from the Department of Dermatology will attend Pemphigus.
Was this article helpful?
YesNo




