Allergy
Blood Diseases
Bone & Joints
Brain
Cancer
Child Care
Cosmetic Surgery
Diabetes
Endocrinology
ENT
Eye
Gen Medicine
General Surgery
Heart
Kidney
Lifestyle
Liver & Digestive
Lung
Men’s Health
Mental health
Physiotherapy
Rheumatology
Skin and hair
Sleep Disorders
Spine
Transplant
Women Health
Thyroid
Vascular Surgery
Rectal Prolapse
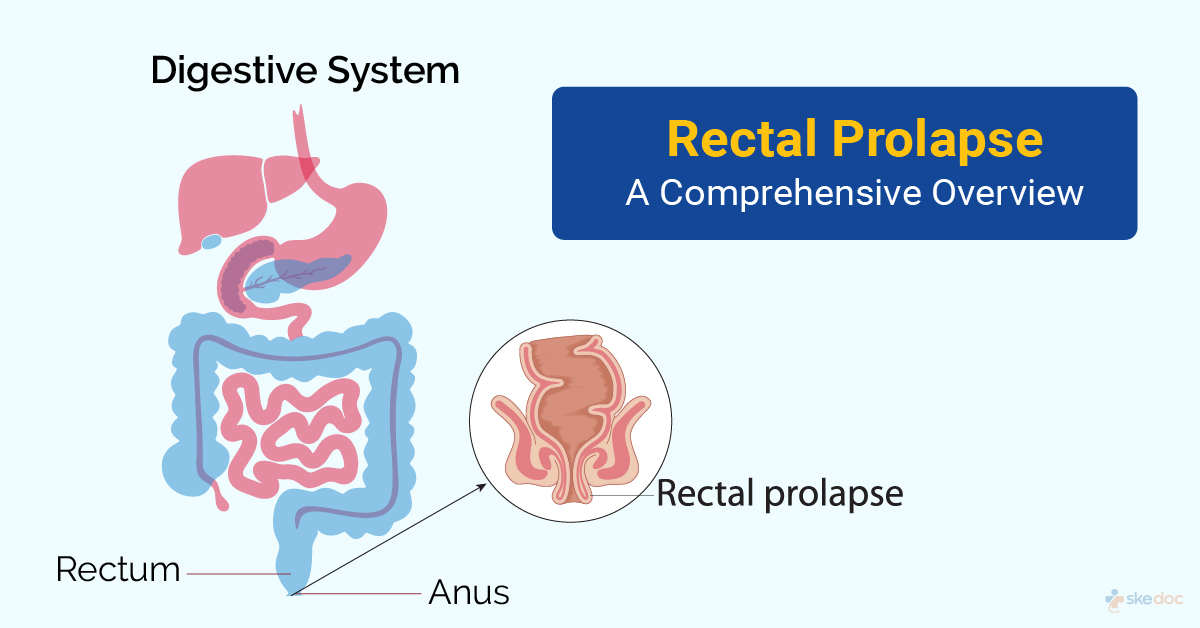
What is Rectal Prolapse?
Rectal Prolapse is a condition where the last part of the large intestine, called the rectum, either partially or fully protrudes through the anal opening. The rectum is the region that is present between the sigmoid colon and the anal canal, and its distal end is the internal anal sphincter.
Is Rectal Prolapse condition a Medical emergency?
Rectal Prolapse is not a medical emergency.
Types
Rectal Prolapse may be of the following types:
- Full-thickness Rectal Prolapse: It is the protrusion of the full thickness of the rectal wall through the anus. It is the most commonly seen Rectal Prolapse.
- Mucosal Prolapse: Only the mucosal lining of the rectum protrudes through the anus
- Internal prolapse (intussusception): It may be a full-thickness or mucosal prolapse, but it does not cross the anal opening.
Causes
The exact cause of Rectal Prolapse is unknown but is thought to be a kind of sliding herniation due to a defect in the supportive connective tissue of the rectal wall or the pelvis. Chronic straining while defecating and constipation are seen in a majority of the cases. This begins as an internal prolapse of the rectal wall and then progresses to a full Rectal Prolapse.
Risk factors
This is usually associated with a weak anal sphincter, separation of the levator ani muscles (levator diastasis), a deep Douglas pouch (the space between the rectum and the back wall of the uterus), poor or weak fixation of the rectum.
Some risk factors for Rectal Prolapse include the following:
- Age - Usually seen after the age of 40 years
- Gender - More common in women
- Pregnancy
- Previous surgeries
- Benign prostatic hypertrophy
- Cystic fibrosis
- Parasitic infections
- Whooping cough
- Pelvic floor dysfunction
- Chronic diarrhea
- Chronic obstructive pulmonary diseases
- Pelvic trauma or lower back injuries
- Spinal tumors
- Multiple sclerosis
- Stool withholding
The risk factors for the collapsed rectal vault in children is due to the presence of a vertical rectum, the mobility of the sigmoid colon, weak pelvic floor muscles, poor mucosa, and submucosa fixation within the rectum. Rectal Prolapse in children is seen below the age of 3 years and is more common in the first year of life.
Symptoms & signs
The symptoms and signs associated with Rectal Prolapse may include:
- History of a protruding mass through the anus
- Mucus discharge through the anus
- Fecal incontinence - as the anus is continuously dilated and stretched
- Constipation or feeling of incomplete evacuation of the bowels
- A feeling of heaviness in the anal region
- Bleeding through the anus
- Altered bowel habits
- Itching around the anus
- A feeling of incomplete evacuation of the bowel - Seen in individuals with intussusception
In the initial stages of a collapsed rectal vault, the protrusion of the rectum happens only after a bowel movement, and the rectum goes back as the individual stands up. As the condition progresses, the protrusion of the rectum begins to occur more often and is associated with straining, coughing, sneezing, or other activities that increase the intra-abdominal pressure. In the late stages of the condition, the protrusion of the rectum is seen with normal activity such as walking, or the protrusion of the rectum may be continuously present.
Investigations
Some investigations that may be done for Rectal Prolapse include the following:
- Laboratory tests:
- CBP & ESR
- Coagulation profile and blood typing
- Liver and renal function tests
- Sweat chloride - To test for cystic fibrosis
- Stool examination
- Imaging tests:
- Barium enema: To identify the presence of any other lesions within the large intestine.
- Colonoscopy: To identify the presence of any other lesions within the large intestine.
- Video defecography: To identify internal Prolapse and to differentiate mucosal Prolapse from full-thickness Prolapse. The individual is asked to defecate on a radiolucent toilet after a radiopaque material, such as barium paste, is instilled into the rectum.
- Rigid proctosigmoidoscopy: It is done to identify any additional lesions affecting the rectum, such as a solitary rectal ulcer
- Anal rectal manometry: To evaluate the anal sphincter muscles; in Rectal Prolapse, there is a decrease in the resting pressure of the anal sphincter and an absence of anorectal inhibitory reflex.
- Sitz marker study: To measure colonic transit
- Pudendal nerve terminal motor latency: To assess any neurologic dysfunction or damage
Diagnosis
A diagnosis of Rectal Prolapse is established based on medical history, clinical evaluation, and results of the investigations done.
Treatment options
The treatment of Rectal Prolapse in adults is usually via surgical interventions, while in children, it may sometimes be managed conservatively by treating the underlying cause.
Medical management
Medical management of Rectal Prolapse is usually as supportive therapy and preparatory therapy before surgical intervention, especially for internal prolapse. It may include:
- Stool softeners: Help decrease strain during bowel movements.
- Polyethylene glycol: An osmotic stool softener that provides a mild laxative effect
- Mineral oil: Lubricates the intestines and allows for easy stool passage
- Lactulose: An osmotic agent that promotes colon movement
- Bulking agents
- Suppositories
- Enemas
- Treatment of the causes of constipation or diarrhea
- Treatment of parasitic infections
Interventional including surgery and indications for surgery
Surgical intervention is the treatment of choice in adults. The choice of Rectal Prolapse surgery depends on the individual's age and general health.
Interventional management of collapsed rectal vault includes may include the following:
- Abdominal Rectal Prolapse Surgery: Associated with a low rate of recurrence but is associated with higher morbidity, and for this reason, they are usually done on young, healthy adults and avoided in older individuals
- Anterior Resection: The sigmoid colon is removed and the rectum is attached to the descending colon so that it can no longer Prolapse.
- Marlex Rectopexy: A mesh or a sponge is used to keep the rectum in place after attaching it to the tail bone.
- Suture Rectopexy: Instead of a mesh or sponge, sutures are used to attach the rectum to the tail bone
- Resection Rectopexy: It is a combination of anterior resection and a market rectopexy
- Perineal procedures: These are associated with shorter hospital stays and lesser postoperative complications and morbidity.
- Anal encirclement: An anal band is placed under the skin around the anus to decrease the size of the anal opening and prevent the rectum from prolapsing. It is currently only done on individuals who are at very high surgical risk or extremely frail and older individuals.
- Delorme mucosal sleeve resection: The prolapsed mucosa is cut and the muscle underneath is sutured in a pleated fashion. It may be done for both small and large Rectal Prolapse.
- Alteimeier perineal recto sigmoidectomy: More suitable for elderly and frail individuals. The recurrence rate after this procedure is high, and recurrence is treated with a repetition of the same procedure.
- Hemorrhoidectomy: This procedure is done if there is a mucosal prolapse
- Perineal stapled prolapse resection: This is considered a fast and safe alternative to most surgical procedures. The recurrence rate after this procedure is extremely high and would require additional surgeries for the management of the recurrence.
- Linear Cauterization: This is usually done for surgical repair in children
Role of Diet/ Exercise/ Lifestyle changes/ Preventive measures
Some measures that may help with the management of Rectal Prolapse include:
- Exercises to strengthen the pelvic floor
- Eating a healthy diet that is rich in fiber
- Avoiding constant straining at school
- Developing healthy bowel habits
Complications
The complications that may be seen with a Rectal Prolapse and surgical intervention for its correction include the following:
- Bleeding
- Infections
- Bowel injury
- Strangulation of the bowel
- Necrosis of the rectal wall
- Altered bowel, bladder, and sexual function
- Leakage of the anastomosis
- Rectocele
- Solitary rectal ulcer syndrome
- Increased risk of cancer
Prognosis
The prognosis of Rectal Prolapse is generally good with early management. Spontaneous resolution may be seen in children. The risk of recurrence is present and can occur even after surgical intervention.
When to contact the doctor or hospital? / How to identify the emergency or complications?
It is advisable to seek medical attention if the symptoms and signs of Rectal Prolapse are noticed.
Indications for hospitalization if required
Hospitalization is not required for Rectal Prolapse unless surgical intervention is warranted.
Suggested clinical specialist/ Departments to consult for this condition
Functional bowel specialists and specialists from the Department of Gastroenterology will treat Rectal Prolapse.
Was this article helpful?
YesNo




