Allergy
Blood Diseases
Bone & Joints
Brain
Cancer
Child Care
Cosmetic Surgery
Diabetes
Endocrinology
ENT
Eye
Gen Medicine
General Surgery
Heart
Kidney
Lifestyle
Liver & Digestive
Lung
Men’s Health
Mental health
Physiotherapy
Rheumatology
Skin and hair
Sleep Disorders
Spine
Transplant
Women Health
Thyroid
Vascular Surgery
Meningitis
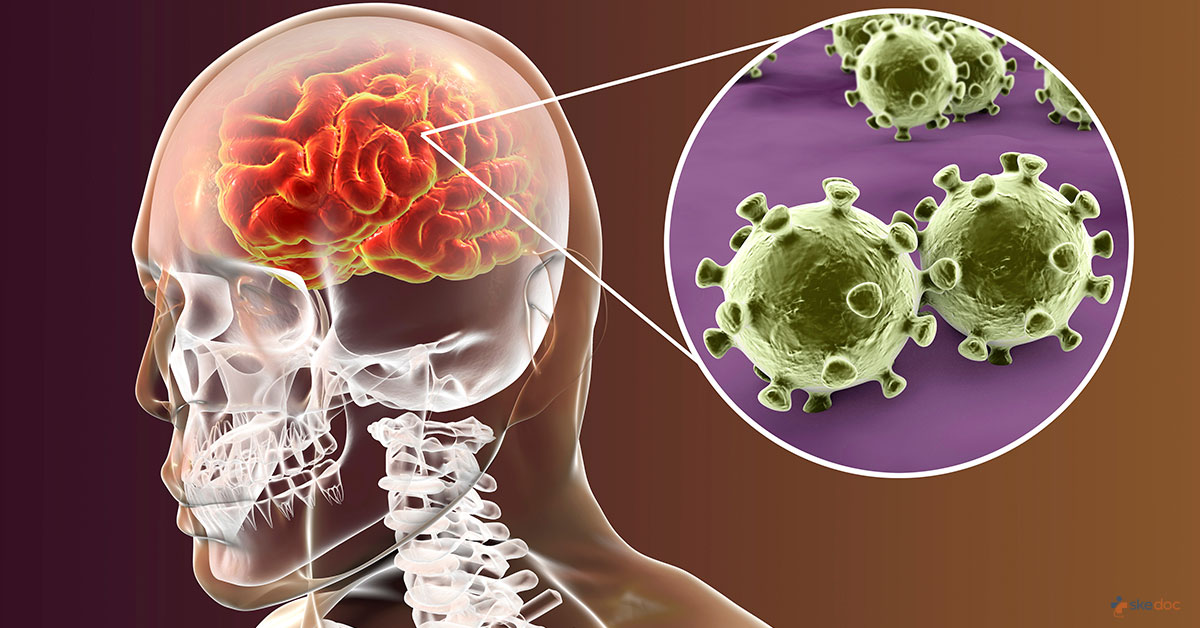
What is Meningitis?
Meningitis is a condition in which there is an inflammation of the meninges of the brain secondary to an infection of the cerebrospinal fluid. The brain and the spinal cord are covered by three protective layers collectively called Meninges. The outermost layer is called the Dura mater and the innermost layer is called the Pia mater. In between these two layers is the Arachnoid mater. A fluid called the Cerebro Spinal Fluid (CSF) circulates within the brain and the spinal cord. It is also present between the Arachnoid mater and the Pia mater.
Is Meningitis a Medical Emergency?
Meningitis that develops over a few hours or a few days is called Acute Meningitis. This is a life-threatening condition and the person must be rushed to the hospital immediately. Any delay in diagnosis or treatment may lead to severe and life-threatening complications.
Types
Based on the duration over which the symptoms evolve, it could be:
- Acute Meningitis: The condition develops within a few hours or days
- Chronic Meningitis: The condition develops over a month. The symptoms remain for over 1 month.
Causes
The two most common causes are Viral and Bacterial infections. Between these two, viral Meningitis is more common while bacterial Meningitis is more dangerous.
Bacterial Meningitis: A bacteria might infect the meninges in several ways:
- After infecting an organ in the body such as the lungs, the germs might spread to the meninges
- An ear infection or a sinus infection can spread to the meninges
- A skull fracture can create a gateway for germs to enter the brain
- In rare instances, the infection might be a consequence of brain surgery
Some common bacteria responsible for this disease are:
- Streptococcus pneumonia: This commonly causes lung infections (pneumonia), ear, and sinus infections.
- Neisseria meningitides: This is found to infect the upper portion of the airways commonly. From there it spreads to the meninges through the blood.
- Haemophilus influenza
- Listeria monocytogenes: This germ is found in dairy products and is particularly dangerous in the case of pregnant women. This is because the bacterium can infect the fetus in the womb as well.
Some common viruses: Responsible for this disease are:
- Enteroviruses: This is the most common class of viruses causing this disease
- HIV
- Herpes simplex virus
- Mumps
- West Nile virus
There is a variant of Meningitis called,
Chronic Meningitis: This infection develops over several weeks or even months.
Mycobacterium tuberculosis: Which causes tuberculosis can also cause Chronic Meningitis.
Fungal Meningitis: It is rare and people with a weak immune system are the ones found to be commonly infected. The fungus most commonly causing this disease is Cryptococcus neoformans which is responsible for chronic Meningitis. Apart from all these, there are some less known causes of this disease. These are:
Non-infectious Meningitis:
- Cancers
- Allergies to medications
- Inflammatory conditions like Sarcoidosis
Risk Factors
Some factors have been identified which can make a person vulnerable,
- Age: Children below 5 years of age are more prone to viral Meningitis while those below 20 years of age are at increased risk of bacterial Meningitis.
- Living environment: Some types of bacterial Meningitis spread rapidly from person to person through droplets. For example, Meningococcal Meningitis. Hence, people living in clusters, like in dormitories or military bases are vulnerable.
- Pregnancy: This is a risk factor, particularly in the case of Listeria Meningitis.
- A weak immune system: People with the following conditions might have weak immune systems:
- AIDS
- Long-standing poorly controlled diabetes
- Cancer
- Taking immunosuppressive medicines after an organ transplant
- Using Steroid medication for a long period
- People who had their Spleen removed
Signs & Symptoms
The common signs and symptoms include:
- High fever
- Severe headache
- A stiff neck
- Repeated episodes of vomiting
- Having an abnormal urge to vomit (nausea)
- Seizures (fits)
- The person may feel confused or abnormally drowsy
- There might be an intolerance to bright light
- A skin rash is also common
The symptoms in an infant are somewhat different:
- The baby might cry uncontrollably
- In contrast to that, some babies show excessive sleepiness
- The muscles and neck might become abnormally stiff
- The infant might refuse to feed
- There might be a bulging fontanel. The soft spots on the baby’s skull where the skull bones haven’t yet fused are called fontanels.
These symptoms are present in addition to a high fever.
Investigations
Some commonly employed diagnostic tests which are done after a thorough clinical evaluation include:
- Laboratory tests:
- CBP & ESR
- Blood Sugar
- Blood Culture with Culture and Sensitivity: To identify the microorganism responsibly
- Polymerase chain reaction (PCR): For viral Meningitis
- Imaging tests:
- The most commonly used methods are CT and MRI scans of the head to identify the sore (inflamed) meninges or any other condition which might be responsible for the symptoms.
- X-Ray of the chest might be needed in some if there is a suspicion of a lung infection which might have been a source.
Spinal Tap: This method, scientifically called Lumbar Puncture, involves the collection of a small sample of CSF and sending it for examination. If a viral infection is suspected, a test called PCR (polymerase chain reaction) is done on the CSF. Bacterial Meningitis can be detected by low glucose levels, high white cell count, and high protein in the CSF.
Diagnosis
A diagnosis of this disease is established based on medical history, clinical evaluation, and results of the investigations done.
Treatment Options
Medical treatment
Each form of Meningitis has a unique treatment approach.
Bacterial Meningitis: Broad-spectrum antibiotics: This targets a wide range of bacteria.
Viral Meningitis: Most cases of viral Meningitis heal by themselves. During this healing process, the person has to be supported through:
- Adequate bed rest
- Plenty of fluids by mouth
- Anti-inflammatory medicines: To control the inflammation of the meninges and to control the headache.
- Corticosteroids: To suppress soreness (inflammation) in severe cases. This ensures there is no swelling of the brain.
- Anticonvulsant Medications: If there are episodes of fits (seizures)
Antiviral medicines are advised only when the Meningitis is caused by the Herpes Simplex Virus.
Other forms of Meningitis: Therapies vary with the scenario. For example:
- Unknown cause of Meningitis: A combination of antibiotics and anti-viral medicines are given until the cause is known
- Fungal Meningitis: Anti-fungal medicines are effective
- Tuberculous Meningitis: Anti-tubercular medicines are given
- Allergic or auto-immune Meningitis: Steroid medicines are beneficial
- Meningitis due to cancer: Underlying cancer has to be treated first
Role of Diet/ Exercise/ Lifestyle changes/ Preventive measures
Preventive measures have been developed and they mainly focus on hygiene and avoiding close contact. This is because several bacterial and viral Meningitis spread through droplets released when a person coughs, sneezes, laughs, kisses, or spits. Similarly, utensils are another common route of spread.
- Regular hand washes: Maintaining clean hands before having food, washing hands after using the toilet, and after handling pet animals lowers the risk of infection.
- Personal hygiene: Avoiding the sharing of personal clothing and utensils is also key in preventing the spread of bacteria and viruses.
- Covering one’s nose and mouth: This has to be practiced without fail while coughing and sneezing to prevent the spread of droplets containing millions of bacteria and viruses.
- Vaccination: Giving vaccines can prevent several forms of bacterial Meningitis. Some commonly used vaccines are:
- Haemophilus influenza type b vaccine (Hib)
- Pneumococcal Conjugate Vaccine (PCV13)
- Pneumococcal Polysaccharide Vaccine (PPSV23)
- Meningococcal Conjugate Vaccine
Complications
The possible complications are:
- Disturbances in memory
- Learning disability, if an infant or a child has been affected
- Hearing difficulties
- Episodes of seizures (fits)
- Difficulty in walking (gait disorders)
- Kidney failure
- A sudden drop in blood pressure to such an extent that it is life-threatening. This condition is called Shock.
- Death may also happen
The possibility of these complications is higher when a person or a child is not diagnosed at the right time and does not receive adequate treatment.
Prognosis
The long-term outcome of treatment is very encouraging, provided, timely diagnosis and appropriate treatment are done. Further, the results are found to depend on age as well. The possibility of death in infants is observed to be higher than that in older children even after adequate treatment. However, the risk of death and the chance of complications are higher in adults.
When to contact the doctor? / How to identify the complications?
Whenever a child or a person is found to have any of the physical features suggestive of this disease immediate medical help has to be taken. A delay in treatment can result in life-threatening consequences.
Indications for hospitalization if required
Hospitalization is needed. The duration of stay is usually for a few days, which might extend depending on the complications.
Suggested clinical specialists/ Departments to consult for this condition
It will be treated by specialists from the Department of emergency medicine and Neurology.
Was this article helpful?
YesNo
Comments





